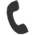Cause, symptoms, diagnosis and treatment

Shoulder bursitis is very common
Bursitis – or inflammation of the bursae – can have a major impact on your daily life. The pain can become so severe you can hardly function. Since bursae are all throughout our bodies, this condition can occur in many joints. The bursae that are most susceptible to inflammation are those in the shoulder, knee, hip, elbow, and ankle. Bursitis is equally common among men and women.
What is a bursa?
A bursa is a type of cushion filled with slimy fluid that lies between the tendons and the bones of a joint and ensures that the joint can move smoothly, without the tendon rubbing against the joint bone. Bursitis is the inflammation of the bursae. Since these protective cushions lie close to the area where the tendon joins to the bone, it is sometimes difficult to distinguish bursitis from an inflamed tendon (tendinitis), because these two conditions cause similar symptoms.
What causes bursitis?

Another form is chronic bursitis. Long-term, mild straining of the bursae, for example due to one-sided straining of a joint during daily activities or sports causes chronic bursitis. This gradually causes the wrong muscular tension on the bursae, increasing pressure on the latter. Chronic bursitis is a rheumatic disease, but generally, bursitis is only temporary.
What are the symptoms of bursitis?
We characterize Bursitis by clear inflammation symptoms. The affected bursa feels swollen and painful, and the area surrounding it can turn red and feel warm to the touch. The tendon has less space to move due to the swelling. If you do try to move around, you may experience intense pain. Moving your joint will be virtually impossible.
How do you diagnose bursitis?
First, your physician will ask you what your symptoms are. If necessary, he can perform an ultrasound to check for signs of inflammation and identify which area is affected. Through an additional examination, your physician will then check whether the inflammation has affected only the bursa or if it is a symptom of a rheumatic disease. Your doctor may also conduct a blood or urine test to exclude the presence of certain rheumatic diseases. Sometimes X-rays are taken to better assess the condition of the joint (cartilage and bone), because if the shoulder is affected, for example, the culprit could also be osteoarthritis, a calcified tendon, ‘frozen shoulder’ etc., which all require a different treatment to bursitis.
How do you treat bursitis?
First, your physician will advise you to rest the affected joint as much as possible. This is usually enough for the inflammation to heal by itself. If you keep moving the joint, your symptoms may persist. Your doctor may suggest that you take acetaminophen, but in certain cases, your physician may prescribe non-steroidal anti-inflammatory drugs (NSAIDs), which often have annoying side effects. However, if you suffer from chronic bursitis, you could therefore opt for a natural alternative, a liquid combination of Green-lipped mussel and Curcumin. In fact, some patients have reported positive results when using these natural anti-inflammatories to treat chronic bursitis. Although it may take longer – up to a few weeks – for you to notice any actual results. Therefore, this treatment is less suitable in case of acute bursitis.
Your physician can also administer a targeted cortisone injection in the joint or bursa, which sometimes yields immediate results. However, usually it does not work, or not sufficiently. Moreover, the pain returns once the effect of the injection has worn off. The physician can also refer you to a physical therapist, who will develop a treatment program aimed at reducing the pain.
Is surgery an option?
If bursitis fails to pass on its own and joint mobility is limited too much, your doctor may suggest keyhole surgery to remove a small part of the bursa. Alternatively, your doctor may suggest traditional open surgery to remove part of the bursa and smooth the underlying joint bone. This type of surgery requires a longer recovery period than keyhole surgery.

Share this page
Tweet

Download for free the booklet ‘Moving without pain’ with a retail value of $6.75 / £4.95.
Any questions? Please feel free to contact us. Contact us.