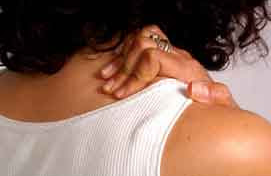
A condition mainly affecting people aged 50 or older
Just like fibromyalgia, polymyalgia rheumatica (PMR) is a rheumatic muscular disease. Patients suffering from PMR have stiff and painful muscles in the neck, shoulder girdle and/or pelvic girdle. PMR generally affects only people aged 50 and older, with women being twice as likely to suffer from this condition than men. In most cases, PMR passes on its own, but it can take two to three years. A small percentage of patients have chronic PMR, with alternating dormant and active cycles.
What is polymyalgia rheumatica?
The name ‘polymyalgia rheumatica’ comes from the Greek ‘poly’ meaning many, ‘myo’, which means muscles and ‘algia’, pain. ‘Rheumatica’ is a reference to rheumatic diseases. In a nutshell, it is a rheumatic inflammatory disease that affects several muscle groups. The inflammation starts in the joint capsule, the tendon sheaths and the bursae surrounding the joints. However, unlike rheumatoid arthritis, this condition does not directly damage the joints. PMR is classified as an auto-immune disorder; simply put, a disease where the immune system attacks healthy cells for no obvious reason. As such, the exact cause of PMR is still unknown. What’s more, blood samples of PMR patients do not show any anomalies. The symptoms of PMR are very similar to those of fibromyalgia, yet they are two distinct conditions. PMR has been definitively categorised as an auto-immune disease, whereas the cause of fibromyalgia is still entirely unknown.
What are the symptoms of polymyalgia rheumatica?
How is polymyalgia rheumatica diagnosed?
To date, no specific tests have been developed to diagnose PMR. That makes it difficult for the GP to identify the disease. Therefore, if you suffer from the symptoms above, you will likely be referred to an internist or a rheumatologist, who will ask you several questions about your symptoms and carry out a physical examination.
An erythrocyte sedimentation rate test (ESR) can measure the sedimentation speed of red blood cells.
If it turns out faster than normal, your physician will know you have an ongoing inflammation process somewhere in your body. Yet this does not conclusively prove you have PMR. To exclude other conditions, the physician will also carry out several other blood tests and usually, he will also take X-rays. If no other disease can be diagnosed through these tests, the physician can conclude you have PMR based on your age, symptoms and ESR. In a nutshell, PMR is diagnosed by exclusion.
How is polymyalgia rheumatica treated?
Prednisone is the medication of choice to treat PMR. This powerful anti-inflammatory and immunosuppressant is a corticosteroid (hormone produced in the adrenal cortex), and for PMR the starting dose is 15 mg daily. Generally, this treatment lasts one to three years, with a gradual decrease of the dose as the symptoms decrease and the ESR improves. If the symptoms suddenly worsen, the dose is once again increased to a level capable of suppressing all symptoms. Sometimes, patients can get by with NSAIDs, fast-acting anti-inflammatory painkillers. The treatment can be supplemented with physiotherapy to decrease stiffness and promote better mobility.
Are liquid Green-lipped mussel and Curcumin an option to treat PMR?
Unfortunately we are unaware of any trials involving PMR patients who have tried this natural alternative to NSAIDs. Various studies have shown that Green-lipped mussel and Curcumin can help fight inflammatory processes, not only in the joints, but all over the body. Theoretically, a liquid combination of Green-lipped mussel and Curcumin could therefore have an effect on the inflammation in the muscles, tendon sheaths, bursae and joint capsules. Should you have any experiences using this treatment as a PMR sufferer, don’t hesitate to let us know.

Share this page
Tweet

Download for free the booklet ‘Moving without pain’ with a retail value of $6.75 / £4.95.
Any questions? Please feel free to contact us. Contact us.