Many people with joint problems (especially osteoarthritis, but also persistent stiffness) use hyaluronic acid, glucosamine, chondroitin or MSM for a shorter or longer period of time hoping that one of these compounds or a combination will relieve the pain in the joints. There are doctors advising against the use of these supplements because the action has not been proven in humans suffering from arthritis. Others don not really have an opinion or are not interested and let their clients use supplements from the ‘if it doesn’t work, it doesn’t hurt’-principle. A few individuals even stimulate the use of these supplements. But how is the real situation regarding hyaluronic acid, glucosamine, chondroitin and MSM?
As explained on the page ‘What is the composition of cartilage?’ hyaluronic acid, glucosamine and chondroitin are an important part of the cartilage matrix. The thought behind the use of these compounds is that the shortage in building material of the damaged cartilage in people with arthritis supplemented by taking large quantities of these compounds.
Hyaluronic acid in arthritis
Hyaluronic acid is often injected in the arthritic joint but can also be taken orally.
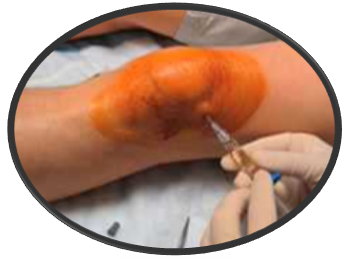
Regarding injections, it is known that they often have a (temporary) effect on the pain in the joint [1,2,3,4], which is not always the case. It seems to be dependent on the kind of hyaluronic acid used. Moreover, some joints and specific joints conditions are less suitable for this treatment [5,6]. In addition, the injection itself can cause a severe inflammatory reaction when the treatment is repeated several times as sometimes happened with the application of Synvisc®, which probably were delayed hypersensitivity reactions [7].
How does such an injection with hyaluronic acid work? A few milliliters of fluid are inserted into the joint with a needle together with the hyaluronic acid, which temporarily supplements the joint fluid. Hyaluronic acid prevents the fluid from leaving the joint immediately because hyaluronic acid had the molecular property to retain the water. Moreover, the molecules are too big to leave the joint without broken down partially first. Therefore, this injection increases shock absorbing of forces on the joint, which might have a relieving effect on the pain. Because hyaluronic acid contributes to the lubrication of the joint, this might temporarily increase. In most cases, this injection needs to be repeated every six months because the injections cannot induce reversal of the inflammatory process [3].
In June 2013, the AAOS, the ‘American Academy of Orthopedic Surgeons’, indicated that injection with hyaluronic acid are no longer recommended in the treatment of arthritis. Therefore, this treatment is no longer reimbursed in the Dutch hospitals since the beginning of 2015.
The oral ingestion of hyaluronic acid did not show many positive results yet. A recent clinical study in patients with knee osteoarthritis showed that it was very difficult to find a significant difference between hyaluronic acid and placebo [8]. However, in this study an important part of the treatment in the hyaluronic acid-group as well as the placebo-group consisted of special knee exercises. Because of this, the placebo group was also better at the beginning of the study. Compared to this, the group that additionally received hyaluronic acid was not much better. Also in horses, orally ingested hyaluronic acid did not result in the expected improvements regarding the symptoms of arthritis [9].
Most likely, there are problems with the absorption from the intestinal tract. In rats, which were administered hyaluronic acid orally, 87-96% of the ingested compound left the body through the urine and feces within 3 hours [10]. In a knee joint, the highest concentration of hyaluronic acid was not measured until 48 hours, which was only 1.7% of all the hyaluronic acid still present in the body [10]. Oral ingestion of hyaluronic acid in knee osteoarthritisis therefore discouraged due to a lack of proof of clinical efficacy and because of a moderate absorption explaining the lack of effect.
Glucosamine and arthritis
Glucosamine-supplements are very popular to use among the Dutch population with arthritic joint complaints. However, as mentioned in the introduction above, a lot of specialists do not see a lot of salvation in this although some glucosamine products are registered as medication. How is that possible?
Glucosamine is a building block for glycosaminoglycan, which in turn form proteoglycans. According to the proponents of glucosamine use extra glucosamine intake can contribute to the construction of cartilage and lubrication molecules with pain relief and more flexibility as a result. Glucosamine compounds such as glucosamine sulphate and glucosamine hydrochloride are relatively well absorbed by the gastro intestinal tract and can reach the joints fairly well [11]. However, glucosamine does far from positively act in all patients even after chronic use.
This was also shown by an important meta-analysis performed by the Bern University (Switzerland) : after combining the results of 10 studies (adding up to 3786 participants!) no significant improvement was found compared to placebo in people with hip- and knee osteoarthritis [12]. At the end of the associated publication it is firmly explained that no relevant pain relief and change in joint space width should be expected from glucosamine and chondroitin and that, although these compounds are safe to use, they should certainly not be reimbursed by health insurance companies [12]. The use of glucosamine seems to be based on a placebo effect in many people.
There are however a limited number of people with starting joint symptoms that experience a relief of the symptoms about three months after glucosamine use although customization occurs after some time when the complaints become worse again [12]. In these people there has probably been a real shortage in cartilage building materials. But when the inflammation as a result of cartilage damage is not inhibited, the newly formed cartilage will eventually be affected causing the complaints to return. Glucosamine can therefore be a temporarily, cheap way out, but it is not active against inflammations and therefore not the solution in the battle against osteoarthritis.
Therefore, also glucosamine is no longer recommended by the AAOS.
Side effects such as headache and nausea sometimes occur with the use of glucosamine. This can be prevented by taking it with a large amount of water or with some food. People with a shellfish allergy have to take into account that a lot of glucosamine products are based on glucosamine from shellfish. For these people, there are also vegetable (and therefore 100% vegetarian) products available.
Chondroitin in arthritis
Just like glucosamine, chondroitin is a building material of glycosaminoglycans. The thought behind the intake of chondroitin is the same as with that of glucosamine. There are also supplements available containing the combination glucosamine-chondroitin, with or without extra MSM, because this is said to be more complete than the separate compounds. The effectivity of these combination preparations did however not appear to be better compared to the individual compounds. This was also the conclusion from the large meta-analysis performed at Bern University discussed before [12]. Therefore, the AAOS does not recommend the use of chondroitin.
MSM and osteoarthritis
MSM (this stands for Methyl Sulfonyl Methane) is a sulfur compound, which is assumed to be able to stimulate the production of cartilage because this contains a lot of sulfur (think about glucosamine sulphate or chondroitin sulphate). From this thought, it is sometimes said that when one wants to ingest chondroitin or glucosamine, the better choice would be glucosamine sulphate or chondroitin sulphate relative to glucosamine hydrochloride.
Indeed, in a systematic review covering all clinical studies applying this sulfur containing compound MSM was found to have a somewhat positive result in people with knee arthritis, although the authors state that no far-reaching conclusion may be drawn because a lot of the reviewed studies do not yet comply with the official reliability requirements [13]. After publication of this review a new study appeared in which MSM a significant, although marginally positive effect compared to placebo [14]. A problem with this last study is that the patients were only followed for three months and therefore long term results are not known [14]. All in all also MSM is a compound that is not unambiguously supported by study results. It is possible to be beneficial in people with starting joint symptoms for some time but MSM does not remove the inflammatory hearth, which also the case with hyaluronic acid, glucosamine and chondroitin.
Read more about the application of hyaluronic acid, glucosamine, chondroitin and MSM in people with rheumatism.
Read more articles in the Knowledge Center.
[1] Vincent, H.K.; Montero, C.; Conrad, B.P.; Horodyski, MB.; Connelly, J.; Martenson, M.; Seay, A.N.; Vincent, K.R. (2013) “Functional pain,” functional outcomes, and quality of life after hyaluronic acid intra-articular injection for knee arthritis. Physical Medicine and Rehabilitation Article in Press (15-4-2013);1934-1482.
[2] Strand, V.; Baraf, H.S.B.; Lavin, P.T.; Lim, S.; Hosokawa, H. (2012) A multicenter, randomized controlled trial comparing a single intra-articular injection of Gel-200, a new cross-linked formulation of hyaluronic acid, to phosphate buffered saline for treatment of osteoarthritis of the knee. Osteoarthritis and Cartilage 20;350-356.
[3] Alberto, M.; Umberto, M.; Emanuele, B.; Bruno, L.; Valentina, G.; Prisco, P.; Mauro, G.; Sandro, T. (2011) Intra-articular injection of hyaluronic acid (MW 1,500-2,000 kDa; HyalOne®) in symptomatic arthritis of the hip: a prospective cohort study. Archives of Orthopaedic and Trauma Surgery 131;1677-1685.
[4] Bannuru, R.R.; Natov, N.S.; Dasi, U.R.; Schmid, C.H.; McAlindon, T.E. (2011) Therapeutic trajectory following intra-articular hyaluronic acid injection in knee osteoarthritis – meta-analysis. Osteoarthritis and Cartilage 19;611-619.
[5] Hsieh, L.-F.; Hsu, W.-C.; Lin, Y.-J.; Chang, H.-L.; Chen, C.-C.; Huang, V. (2012) Addition of intra-articular hyaluronate injection to physical therapy program produces no extra benefits in patients with adhesive capsulitis of the shoulder: a randomized controlled trial. Archives of Physical Medicine and Rehabilitation 93;957-964.
[6] DeGroot III, H.; Uzunishvilli, S.; Weir, R.; Al-omari, A.; Gomes, B. (2012) Intra-articular injection of hyaluronic acid is not superior to saline solution injection for ankle arthritis. The Journal of Bone and Joint Surgery. American Volume 94;2-8.
[7] Monfort, J.; Lisbona, M.P.; Gimenez-Arnau, A.; Iglesias, M.; Llorente-Onaindia, J.; Benito, P. (2013) Immunoallergic reaction following intraarticular injection of high molecular weight hyaluronic acid. Joint Bone Spine Article in Press (15-4-2013).
[8] Tashiro, T.; Seino, S.; Sato, T.; Matsuoka, R.; Masuda, Y.; Fukui, N. (2012) Oral administration of polymer hyaluronic acid alleviates symptoms of knee arthritis: a double-blind, placebo-controlled study over a 12-month period. The Scientific World Journal 2012;Article ID 167928.
[9] Carmona, J.U.; Argüelles, D.; Deulofeu, R.; Martínez-Puig, D.; Prades, M. (2009) Effect of the administration of an oral hyaluronan formulation on clinical and biochemical parameters in young horses with osteochondrosis. Veterinary and Comparativ Orthopaedics and Traumatology 22;455-459.
[10] Balogh, L.; Polyak, A.; Mathe, D.; Kiraly, R.; Thuroczy, J.; Terez, M.; Janoki, G.; Ting, Y.; Bucci, L.R.; Schauss, A.G. (2008) Absorption, uptake and tissue affinity of high-molecular-weight Hyaluronan after oral administration in rats and dogs. Journal of Agricultural and Food Chemistry 56;10582-10593.
[11] Persiani, S.; Rotini, R.; Trisolino, G.; Rovati, L.C.; Locatelli, M.; Paganini, D.; Antonioli, D.; Roda, A. (2007) Synovial and plasma glucosamine concentrations in arthritis patients following oral crystalline glucosamine sulphate at therapeutic dose. Osteoarthritis and Cartilage 15;764-772.
[12] Wandel, S.; Jüni, P.; Tendal, B.; Nüesch, E.; Villiger, P.M.; Welton, N.J.; Reichenbach, S.; Trelle, S. (2010) Effects of glucosamine, chondroitin, or placebo in patients with osteoarthritis of hip or knee: network meta-analysis. British Medical Journal 341;c4675.
[13] Brien, S.; Prescott, P.; Bashir, N.; Lewith, H.; Lewith, G. (2008) Systematic review of the nutritional supplements dimethyl sulfoxide (DMSO) and methylsulfonylmethane (MSM) in the treatment of arthritis. Osteoarthritis and Cartilage 16;1277-1288.
[14] Debbi, E.M.; Agar, G.; Fichman, G.; Bar Ziv, Y.; Kardosh, R.; Halperin, N.; Elbaz, A.; Beer, Y.; Debi, R. (2011) Efficacy of methylsulfonylmethane supplementation on arthritis of the knee: a randomized controlled study. BMC Complementary and Alternative Medicine 2011 11;50.

Share this page
Tweet

Download for free the booklet ‘Moving without pain’ with a retail value of $6.75 / £4.95.
Any questions? Please feel free to contact us. Contact us.